Why preventing food insecurity will support the NHS and save lives

Rising rates of food insecurity are a national crisis and put the most vulnerable at risk. With the scale of increases in the cost of healthy food choices, there is a risk of devastating and long-lasting impacts on people’s health and wellbeing. This in turn impacts the demand for NHS services to treat the acute and chronic conditions caused by hunger and unhealthy diets.
As the increasing rate of food insecurity is largely being driven by the cost-of-living crisis, government policies need to support those most at risk in order to address the root cause.
Key points
- Food prices have risen by 14.6 per cent in the last year, the highest rate of increase since 1980.
- Combined with other pressures on household budgets, such as increasing energy bills and a ten per cent reduction in the real-terms value of benefits, this has resulted in one in four households with children experiencing ‘food insecurity’ in September 2022, which means being unable to afford sufficient or nutritious food.
- Food insecurity is linked with malnutrition, obesity, eating disorders and depression. Obesity is now overtaking smoking as the number one cause of preventable death in England and Scotland.
- Given the scale of increases in the cost of healthy food choices, if current circumstances continue we will see devastating and long-lasting impacts on people’s health and wellbeing.
- Primary-school-age children from England’s most deprived areas are around five times more likely to be living with severe obesity than those in the least deprived areas. This has a negative impact on a child’s life chances.
- The NHS will pay the price, now and into the future, for treating the acute and chronic conditions caused by hunger and unhealthy diets. Spending on obesity is forecast to rise to £9.7 billion per year by 2050 and malnutrition is estimated to cost the NHS £19.6 billion per year.
- Integrated care partnerships (ICPs) present an opportunity to develop strategies to tackle food insecurity and take collaborative action at system, place and neighbourhood level. This will reduce health inequalities and provide a return on investment by decreasing the demand that food insecurity places on the healthcare system.
What is food insecurity and what does it look like in the UK?
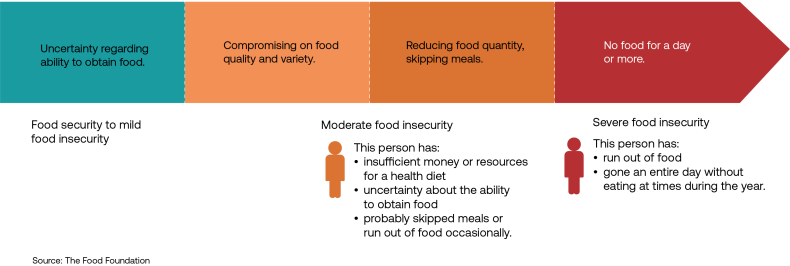
The Food Foundation defines food insecurity as being unable to reliably access sufficient, affordable and nutritious food. It is experienced at differing levels of severity, measured on the Food Insecurity Experience Scale. High levels of insecurity can result in the need for food banks and in persistent hunger: neither should have a place in modern Britain.
The inability to access healthy, nutritious food negatively affects our physical and mental health across the whole life course, including development, wellbeing and ability to thrive. A recent study found that it is three times more expensive to get the energy we need from healthy foods, but calorie-dense, processed foods often lack other important nutrients. This means health conditions resulting from poor diets are more common in lower-income groups and are associated with ‘considerable, unacceptable costs to the NHS and UK economy.’ (Parliament.uk)
Data from the Food Foundation’s food insecurity tracker showed that in September 2022, an estimated 18.4 per cent of UK households (9.7 million adults) had experienced moderate or severe food insecurity in the past month. This is a 9.6 percentage point increase from January this year. One in four UK households with children (4 million children) experienced food insecurity this September. There is significant regional variation in food insecurity, and the highest prevalence exists in the north east of England, where 27.8 per cent of households experienced food insecurity in the last month.
What is driving the current levels of food insecurity?
The main driver of food insecurity for British households is the rapidly rising cost of food. Inflation in the cost of household goods reached 10.1 per cent in July 2022 and the Bank of England has forecast continued increases. Food prices have been rising even more quickly than the headline rate. They were 14.6 per cent higher in the year to September 2022 based on the official CPI measure of inflation, up from 12.6 per cent in July 2022, which is the highest rate of increase since comparable records began in 1980 and up from 13.1 per cent in August [ 1 ]. The average food shop is forecast to rise by £643 annually, at a time when families also face higher costs for energy, transport and housing.
The impact of inflation, and consequently the risk of food insecurity, is not faced equally. Research from the Institute for Fiscal Studies shows that the lowest income households face higher rates of inflation. In April this year, the lowest income households faced an inflation rate three per cent higher than the most well-off households and this is expected to rise to seven per cent higher in October. This higher rate of inflation is driven by lower income households spending a larger proportion of their overall income on energy bills. These have doubled in the last 12 months so that the average household will pay £2,500 per year on energy from October 2022, compared to £1,277 in October 2021.
With other cost pressures on household budgets, families will have limited capacity for choice about the nutritional value and/or quantity of the food they are able to access. This has meant that households in areas with the highest rates of deprivation, families with a low income (particularly those with young children), people with disabilities, older people, and undocumented migrant families are at greater risk of food insecurity. A 2022 study of undocumented migrant households in Birmingham found that 96 per cent were food insecure.
Eight per cent of the most deprived areas of the UK are food deserts, where there is no access to healthy and affordable food. The high price of fuel and associated increased transport costs will mean people living in food deserts will be more likely to remain close to home, eating less than they need, or eating food with low nutritional value.
Rising energy bills mean that cooking costs have also increased. Food banks have reported that users are having to reject nutritious options such as root vegetables and potatoes because they cannot afford the energy costs to boil them. A recent campaign from the supermarket chain Iceland and energy supplier Utilita calculated annual cost savings of over £200 when consumers switch to microwaves and air fryers, rather than using the oven.
Increasing numbers of people are having to use food banks. Over 25,000 people asked Citizens Advice for help accessing food banks and charitable support in August 2022, which is a 171 per cent increase from August 2020. Around one third of requests for support (8,000) came from people approaching Citizens Advice for the first time.
What does this mean for people’s health and wellbeing?
Unhealthy diets increase the risk of chronic illnesses such as diabetes, cardiovascular disease, certain cancers and the likelihood of obesity. Food insecurity can also lead to people avoiding eating. Going hungry, even just a few times, is linked to decreased immunity and poorer mental and physical health, and can cause malnutrition, heart disease and fatigue.
The mental health impact of food insecurity is striking. Participants in a survey from The Money and Mental Health Policy Institute described the effect of the cost-of-living crisis on their mental health:
“[I feel] more depressed. Don't eat as much. Panic when food shopping in case I spend too much.”
“For us, this really could be the straw that breaks the camel’s back. Never before in my life have I had to choose between having warmth and being able to put food on the table. Now that is very much a reality... Finances have always been tough, but nothing like they are now.”
Almost half of respondents to the survey in May 2022 had reduced the number of meals they ate in a day and cut spending on essentials like food – and food price inflation has increased by 4 per cent since then. Respondents with recent experience of mental health problems also reported feelings of anxiety, depression and hopelessness as a result of the rising cost of living.
Children and teenagers
Children and young people in the UK are affected by food insecurity, particularly following the COVID-19 pandemic, which contributed to increased financial and food insecurity in households with children[ 2 ]. Research from the Food Foundation found that in September this year, 4 million children lived in households that were experiencing food insecurity. This is creating demand on the healthcare system now: in Scotland, child admissions to hospital for malnutrition doubled in the last year.
In 2022, 1.9 million (22.5 per cent) of children and young people were eligible for free school meals; an indicator of food insecurity. Despite this high number, the Child Poverty Action Group has raised the alarm that restrictive criteria mean that as many as one in three (800,000) school-age children living in poverty are not eligible. Others are dissuaded from claiming their free school meal because of stigma and, in an upcoming report from charity Chefs in Schools, some headteachers report children ‘pretending to eat out of an empty lunchbox’ because there is no food at home.
Arriving at school hungry means children are less able to concentrate, risk falling asleep in class and have problems socialising. Food eaten at school makes up 17 per cent of what a child in primary school eats in a day, and our eating habits and patterns are formed in our early years, so expanding the availability of nutritious, free school meals represents a real opportunity to reduce nutrition-related inequalities. However, free school meals are not enough. Growing up in poverty has lifelong implications for wellbeing and life chances and preventing this should be a key societal goal.
Food insecurity also increases the risk of obesity. The prevalence of childhood obesity in children in reception and year six increased by about 5 percentage points between 2019 and 2020. There has also been a widening of inequalities associated with severe childhood obesity. Children in reception who live in England’s areas with the highest levels of deprivation are around four times more likely to be living with severe obesity than those areas with the lowest levels of deprivation. By year six, this rate climbs to six times more likely.
Recent research has also shown an association between food insecurity and certain eating disorders, particularly binge-eating disorder and bulimia nervosa. Low income, marginalised groups living with food insecurity had significantly higher risks of eating disorders. The number of children and young people in England referred to eating disorder services was three times higher at the start of 2022/23 than pre-pandemic. NHS England says this rise could be attributed to the unpredictability of the COVID-19 pandemic, feeling isolated, disruption to routines and experiences of loss and uncertainty.
Adults, including older people
COVID-19 has intensified the financial hardship faced by low income households and increased the risk of food insecurity.
There were more than one million hospital admissions due to obesity than before the pandemic in 2019/20. These admissions were over three times more likely to be in the country’s most deprived areas. Over 40 per cent of households in receipt of Universal Credit are food insecure and over 60 per cent of people who referred to food banks in August 2022 had a disability or long-term health condition, which is around three times the rate of the general population.
As well as worsening financial hardship, COVID-19 served to widen racial inequalities in terms of food security. Research from the Food Foundation found that extremely clinically vulnerable people are more than twice as likely than average to be food insecure. The study also found that since the pandemic, inequalities in food insecurity have widened between people from black, Asian and ethnic minority groups and white British ethnic groups, with more than twice as many black, Asian and ethnic minority households having experienced food insecurity than white households in the six months up to January 2021.
Older people are particularly vulnerable to the effects of malnutrition. The Malnutrition Task Force recently calculated that as many as 1.3 million older people are malnourished or at risk of malnutrition. Age UK found that 1.4 million older people have been eating less, and 3.7 million older people have been unable to eat healthy and nutritious food since the start of the COVID-19 pandemic. In older people, malnutrition is associated with long-term conditions such as problems swallowing, cancer, chronic obstructive pulmonary disease, dementia and physical disability, as well as muscle wastage, which increases risk of falls.
What is the impact on the NHS and what are health and care organisations doing to help?
Greater food insecurity could create unmanageable pressure on already stretched NHS budgets. The NHS will pay the price, now and into the future, for treating the acute and chronic conditions caused by hunger, inadequate nutrition and unhealthy diets.
Recent research suggests that obesity has overtaken smoking as the number one cause of preventable deaths in England and Scotland. Rising rates of obesity mean rising NHS costs to treat the disease. In 2014/15, the NHS spent £6.1 billion on treating obesity related ill health. This is forecast to rise to £9.7 billion per year by 2050. In addition, malnutrition is estimated to cost the NHS in England £19.6 billion per year, and the cost of treating a malnourished patient is two to three times more than a non-malnourished patient.
Integrated care partnerships (ICPs) present an opportunity to develop strategies to tackle food insecurity and take collaborative action at system, place and neighbourhood level. This will reduce health inequalities and provide a return on investment by decreasing the demand that food insecurity places on the healthcare system.
Our members are committed to supporting their staff and communities to cope with the increased cost of living.
#OneSlough
To support patients and communities, #OneSlough, a partnership comprising stakeholders and partners including Frimley ICS, Slough Borough Council and the voluntary, community and social enterprise (VCSE) sector, is developing programmes to alleviate food insecurity in the borough. A number of community pantries are opening across the area in the coming months. The same team is also partnering with the Meals from Marlow scheme that, during COVID-19 lockdowns, provided free hot meals to community groups who then distributed them through their own networks. This meal delivery service is being revitalised in Slough, and the team is working with community groups and their primary care networks to investigate if GPs can refer patients who need emergency help with meals.
Morecambe Bay NHS Foundation Trust
Morecambe Bay NHS Foundation Trust provides care packages on discharge to patients who require an extra level of support. Ward staff assess whether the patient might not have food in at home due to food insecurity, a lack of nearby relatives, or because of a long stay on the ward. The patient is sent home with a care package so that they are not discharged to empty food cupboards. The package includes tea or coffee, milk, bread, butter, jam, a tin of soup or beans, and cereal. This care package is charged to the ward’s budget and costs are kept low thanks to partnerships with the food suppliers. The trust’s catering team is also in the process of developing a set of low-cost, nutritious, simple recipes to give to patients on discharge, because of the mental and physical health benefits of home cooking.
Nottingham and Nottinghamshire ICS
Nottingham and Nottinghamshire ICS recognises that its staff and local communities are facing an unprecedented combination of pressures and are committed to collective action at every level where the NHS can play a role to mitigate the health impacts of the rising cost of living. The ICS’s approach is to ensure that NHS providers and local authority teams in the system makes every contact count by enquiring about access to food and heating, and their place-based partnerships are supporting access to food banks and other support offers through partnerships with the VCSE sector. Primary care networks in the area identify and support vulnerable households through proactive signposting, and work with the VCSE and local authority public health teams to provide support mechanisms where available, supported by the integrated care board (ICB) and place-based partnerships.
Southwark Council
Partnership working will be crucial to creating food-secure communities. Southwark Council is tackling food insecurity through a co-ordinated borough-wide approach with key partners. The focus is on prevention, resilience and tackling wider determinants of food insecurity, assessing need and service provision through its three-tier response: solving structural and policy issues that cause food insecurity (access to affordable, healthy food); building resilience (empowering and upskilling people); and crisis provision (emergency food aid). More examples of local government programmes tackling food insecurity can be found on the Local Government Association’s website.
As well as supporting patients and communities, NHS Confederation members have also developed initiatives to support staff from the rising cost of living.
Royal Orthopaedic Hospital NHS Foundation Trust
The Royal Orthopaedic Hospital NHS Foundation Trust has an on-site food bank where colleagues can access food in a discreet area of the hospital. The trust provides carrier bags so that staff can fill up a bag and no one needs to be aware. There is also signposting to the local food bank and services for individuals and families, which are near the hospital. Staff are encouraged to contact them, as further ongoing support can be offered.
Newcastle Upon Tyne NHS Foundation Trust
Newcastle Upon Tyne NHS Foundation Trust offers discreet meal cards for staff who may be unable to prioritise funds, to enable them to eat and drink while at work. Chaplains and the catering team can issue the credit-card-sized card, which is titled ‘staff loyalty card.’ Cards are returned at the end of use and can be exchanged, and further support sought. This is funded by the Newcastle Hospitals Charity.
More examples of support for health and care staff from member organisations are available on the NHS Employers website.
What more can be done? Our asks of national and local policymakers
Rising rates of food insecurity are a national crisis and put the most vulnerable at risk. This must be addressed at place, system and national level through a focus on prevention and resilience building, rather than crisis management. As the increasing rate of food insecurity is being driven largely by the cost-of-living crisis, government policies need to support those at most risk of financial insecurity in order to address the root cause.
Calls to government
Expanding the eligibility for free school meals to all children from households in receipt of Universal Credit was recommended in 2020’s independent National Food Strategy (costed at an additional £670 million per year). The government’s response promised to keep eligibility for free school meals under review. The rollout of universal free school meals began this year for primary school children in Wales.
Given that one in four UK households with children (4 million children) experienced food insecurity in September 2022, and in Scotland, child admissions to hospital for malnutrition doubled in the last year, the NHS Confederation urges the government to expand the eligibility of free school meals and breakfast clubs to all households with low incomes in the UK. This intervention aims to reduce stigma, save families around £400 per child annually, and give all children the best chance to eat a healthy diet. In turn, this will reduce pressure on the NHS.
Food insecurity negatively affects the nation’s health and the NHS’s budget. It is therefore necessary to provide targeted support for those most at risk, to ensure household incomes do not fall below a liveable threshold. One way of doing this is ensuring that benefits rise in line with inflation. The lowest income households face an inflation rate around seven per cent higher than the most well-off households.
Although then-Chancellor Rishi Sunak committed to uprate benefits in line with inflation next April, the current government has not yet confirmed if this commitment will be upheld and it has been suggested that instead, benefits could be uprated in line with earnings. Under the established system, benefits are uprated each April in line with inflation the previous September which, although not yet announced, is likely to be around ten per cent. The chair of the Work and Pensions Committee wrote to the Chancellor Kwasi Kwarteng on 3 October 2022 warning that failing to uphold the commitment would risk pushing ‘countless families further into crushing poverty.’ Recent research from the Legatum Institute estimated there would be 450,000 more people living in poverty in 2023-23 if benefits were uprated in line with earnings, rather than inflation.
The current system of uprating benefits in April in line with inflation the previous September has resulted in benefits losing just over ten per cent of their real-terms value over the course of the year. This amounts to a huge reduction in household budgets and likely contributed to the record high number of people (25,000) who approached Citizen’s Advice to access food banks in August 2022. The Institute for Fiscal Studies has recommended updating this to a system that uses a more current measure of inflation.
The impact of global determinants on food insecurity requires a cross-government approach to policymaking that considers the social, political, economic and commercial determinants of food insecurity. Or, as it is sometimes referred to, adopting a ‘health in all policies’ approach to policymaking. National action should form part of the strategic programme of work undertaken by parliament’s Food Security Inquiry and aim to tackle not only the causes of food insecurity, but also wider health inequalities such as obesity that if left unaddressed will continue to divide the health of the nation.
Considerations for local systems
- Consider food insecurity as a key determinant of health when creating ICP and ICB strategies.
- ICPs present an opportunity to develop strategies to tackle food insecurity at system, place and neighbourhood level. This will reduce health inequalities and provide a return on investment by decreasing the demand that food insecurity places on the healthcare system. Examples of actions members are taking to tackle food insecurity are available on the NHS Confederation’s cost-of-living web pages.
Considerations for NHS England and the Office for Health Improvement and Disparities
- System-wide resources and education on food insecurity should be made available to health and care practitioners across the NHS, local government and the voluntary, community and social enterprise sector to increase awareness of food insecurity.
- Prioritise the development of screening tools specific to the UK population that can be implemented in clinical practice, serving as a prompt to initiate conversations on food insecurity. This should follow the lead of the Royal College of Paediatrics and Child Health, which has issued paediatricians with detailed advice on how they can help households in poverty.
If you have any questions or would like to engage with the NHS Confederation’s cost-of-living work, please contact Ruth Lowe at ruth.lowe@nhsconfed.org.





