Addressing vaccine hesitancy in different ethnic communities
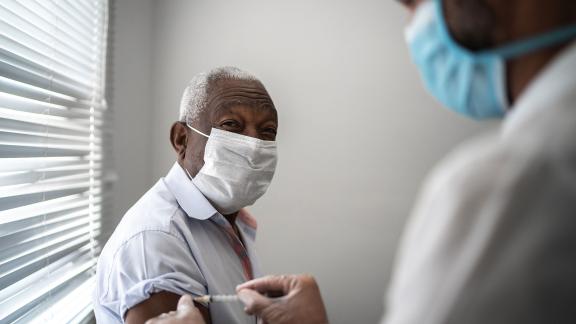
Cheshire and Merseyside Health and Care Partnership used insight gained from a four-stage programme to understand the impact that COVID 19 was having on ethnic minority communities, and work with the different communities to understand the causes of the hesitancy. This programme of work, which entailed partnership working between multiple agencies as well as with the various communities, led to a significant increase in vaccine uptake in just four months.
Key benefits and outcomes
- Increased vaccination uptake in ethnic minority communities from 0.66 per cent in February 2021 to 38.35 per cent in May 2021.
- Valuable insight gained into how COVID-19-related messages are perceived and acted on by different communities, which has been shared nationally.
- Working closely with different partners helped to quickly build trust.
- The campaign successfully influenced a long-standing cultural shift in NHS communication and engagement with ethnic minority groups.
What the organisation faced
In the closing months of 2020, there was distrust among different ethnic minority groups in the Cheshire and Merseyside area in vaccine messaging. Daily reporting in the press and social media of the significantly high and disproportionate number of deaths of ethnic minority NHS staff and other key workers exacerbated the lack of trust. Ethnic minority groups were also experiencing disproportionate deaths in their own communities and felt isolated and ignored.
The genuinely held concerns at the root of the vaccine hesitancy were underpinned by uncertainty and combined with some ambivalence. Some of these stemmed from individual and group experiences of healthcare and others related to feeling disenfranchised and lacking access to credible information. A ‘one-size fits all’ approach simply wouldn’t work.
What the organisation did
In this emergency scenario, quick and responsive public health thinking was essential. A better understanding of the cultural, behavioural and religious aspects that influence health and care and that were influencing vaccine hesitancy was a priority, so a campaign was planned that outlined clear recommendations on how the NHS needed to work in conjunction with GPs, local community organisations and faith groups on a programme of engagement to build trust.
Funding was quickly secured for the initial research from a consortium of partners including NHS England and NHS Improvement (NHSEI), Public Health England (PHE) and Cheshire and Merseyside’s directors of public health. The steering group was made up of representatives from local authorities, the NHS, PHE and the voluntary and community sector.
A unique interactive tool was developed during stage one of the campaign which used school census data, indices of multiple deprivation (IMD) and other data sources to refresh the outdated census and give a current understanding of each postcode’s ethnic communities, to see exactly where different ethnicities lived and segment each group into higher and lower deprivation clusters.
The programme engaged with 636 residents across all 16 ethnic groups in a detailed quantitative research study.
GPs from the different communities were closely involved in the research and this contributed to uncovering a myriad of reasons for vaccine hesitancy. These included concerns over leaving the house, travel and access could lead to catching the virus. There was also a high level of concern over the fact the vaccines had been produced so quickly, as well as the vaccine’s efficacy and side effects. Research showed the gypsy, Irish, Bangladeshi, and some black/mixed groups were the strongest rejecters of the vaccine (over a fifth).
The programme needed the right agencies to start the work, so early on (in October 2020) an agency was commissioned that could speak in the languages of some of the key communities. This meant that the programme could engage with ‘seldom heard’ groups, in particular with people for whom English was not their first language.
However, it was partnership working that entailed the right messages reached the right people. Directors of public health were instrumental in connecting teams to the right people to cascade the information out. Although health teams were closely involved in delivering the vaccine itself, the voluntary sector also played a key role in reaching out to lots of community groups – mosques, mental health teams and other services were all involved. Each group was given the tools and materials to deliver their own tailored communications.
Results and benefits
The engagement programme’s quantitative research study (achieved through multiple recruitment methods, including an online panel, social media, public relations, community outreach and local businesses engagement), helped capture valuable insight into what the programme could be doing to improve NHS communication and interventions with these communities. This was no mean feat given that for 35 per cent of respondents, English was not their first language.
Teaming up with local ethnic representatives to directly address the main barriers identified, resulted in an impressive increase in uptake of vaccination. In February 2021, only 0.66 per cent of minority ethnic individuals who were eligible came forward for vaccination, but this increased incrementally to 13.10 per cent in March, to 30.58 per cent in April and 38.35 per cent in May.
These impressive results have been shared nationally and the campaign insights are widely viewed as a trailblazer for significantly contributing to a cultural shift in NHS communication and engagement with ethnic minority groups.
The fresh insights uncovered will leave a lasting legacy and provide a benefit not only in Cheshire and Merseyside, but for organisations across the country to learn more effective ways to engage with ethnic communities and adapt services and interventions accordingly.
Overcoming obstacles
Broad assumed hesitancy would have been a barrier, so the programme lead, Edna Boampong, identified that fast tracking the programme would gain a quick and essential understanding of the nuances within every different community, as well as the cultural, behavioural and religious aspects that influence health and care.
For example, vaccine hesitancy campaigns across the region initially targeted predominantly the Asian community, but within the Cheshire and Merseyside area there were differences within all ethnic communities.
The research showed there was less vaccine hesitancy in the Indian community than the Pakistani community and more hesitancy in African groups than the Afro Caribbean communities. A recognition of these nuances was essential.
This meant developing effective strategies and messages for all the different groups within different ethnicities and in turn recognising their differing concerns and issues.
Transport was an additional common barrier to communities receiving the vaccine, but by ensuring the vaccine was available in areas where people went (such as shopping centres, churches and mosques) this made it easier to boost uptake.
Takeaway tips
- The campaign’s strong and authentic public health messaging made it easier to utilise the skills of a variety of people across teams and communities to reach the right people.
- Using each teams’ knowledge and expertise within their own areas and communities really helped to reach the intended audience and enable the huge behavioural shift.
- The campaign’s use of real people from within hesitant communities to deliver the vaccine messages was important in engendering trust. It wouldn’t have been as effective if celebrities or politicians were brought in to do the work.
- Instead of expecting people to go to health centres to get their vaccine, the vaccine was delivered in more accessible places, where the communities lived and worked.
Further information
For further information about the work in this case study, please email
Edna Boampong, project director: e.boampong@nhs.net
or
Christine Hughes, executive director of communications and engagement: Christine.hughes19@nhs.net
This page is included in our collection of case studies and resources on our vaccination hub, produced in partnership with ABPI.



