Hardwiring a population health improvement approach within local health and care systems

Ensuring that a population health improvement lens is embedded within local integrated care systems is critical if they are to achieve their shared purposes of improving outcomes, tackling inequalities, enhancing productivity, making best use of resources, and strengthening local communities at a system and place level.
As the greatest public health crisis in more than a generation, the COVID-19 pandemic has tested the limits of public health systems across the globe. Some systems have drawn criticism, while others have been praised, but all have been challenged by the cunning novel virus.
In England, the advent of statutory integrated care systems (ICSs), conceived to improve population health and reduce health inequalities, present an opportunity to hardwire public health approaches into the health and care service’s DNA.
But what can be done to ensure a strong role for public health in ICSs? And what opportunities do changes to the public health architecture afford? For healthcare leaders, public health experts, local government leads and the healthcare industry, the evolving landscape presents fertile ground. This was the focus of discussion at a recent NHS Confederation roundtable, hosted by Novartis Pharmaceuticals UK Ltd.
Harnessing the zeitgeist
Given that tackling health inequalities and improving population health outcomes is currently the zeitgeist of political parlance, health and care leaders at the roundtable event felt that the changes to public health architecture both at the national and local levels provide an immense opportunity to address the systemic health inequalities that exist.
…public health teams within local authorities have been a crucial component in the response to the COVID-19 pandemic.
For local system leaders, the learning from the COVID-19 pandemic vaccination programme has shown how the development of rapid feedback loops and accountability allowed them to innovate and adapt delivery care models with clear outcomes that need to be established across other health improvement programmes. For example, high vaccination rates across communities.
Participants expressed that public health teams within local authorities have been a crucial component in the response to the COVID-19 pandemic. However, directors of public health have been encountering numerous challenges of workforce capacity and funding within local systems.
For a local health and care system to have a public health perspective within all its partners and components, discussion revolved around the need to extend involvement to include the NHS and wider stakeholders, such as voluntary and community groups.
Finally, data integration was debated, and how integrated systems may achieve a true shift in health and care delivery by focusing on population health outcomes and not other process outcomes.
Key action points
Overall, a number of key actions emerged from the day’s discussions:
- The NHS Confederation to facilitate discussion on challenges, enable greater understanding, and share best practice of embedding public health and population health management across the NHS, national and local public health, and ICSs.
- ICSs to develop:
- effective communication channels between national and local public health systems
- establish faster feedback loops to report on outcomes
- enhance public health workforce capacity and capability
- improve cross-sectoral communication and transformation
- deliver data-driven integration to incentivise health improvement outcomes and not activity
Now is the opportunity to get ICSs structured in a way that focuses on the wider social determinants of health and operates through a public health lens, to deliver equitable outcomes for their populations.
Going forward, the NHS Confederation will continue to support local health and care system leadership through facilitating conversations between local and national public health systems.
This infographic captures the discussion and visually demonstrates the current journey and the changes required to embed public health into ICSs.
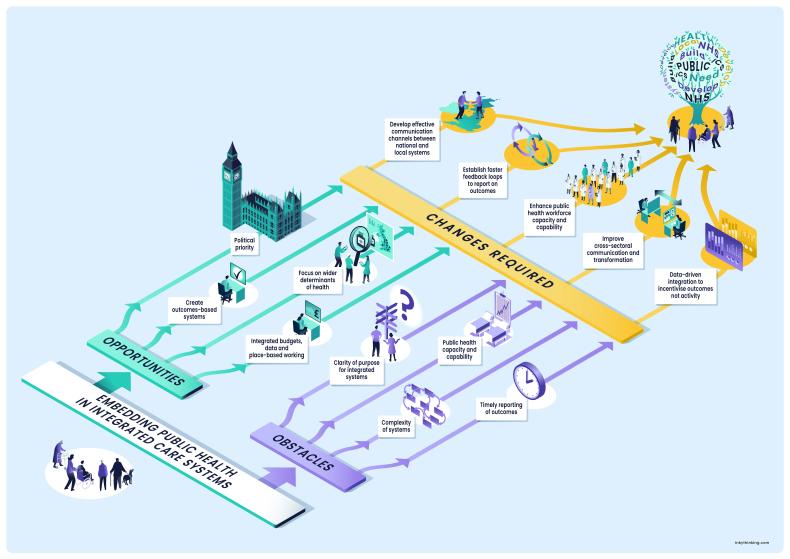
Meeting notes summarising the full session are also available.
Hashum Mahmood is senior policy adviser for population health at the NHS Confederation.
This roundtable discussion was sponsored by Novartis Pharmaceuticals UK Ltd. Editorial control of the content remains with the NHS Confederation.



