COVID-19
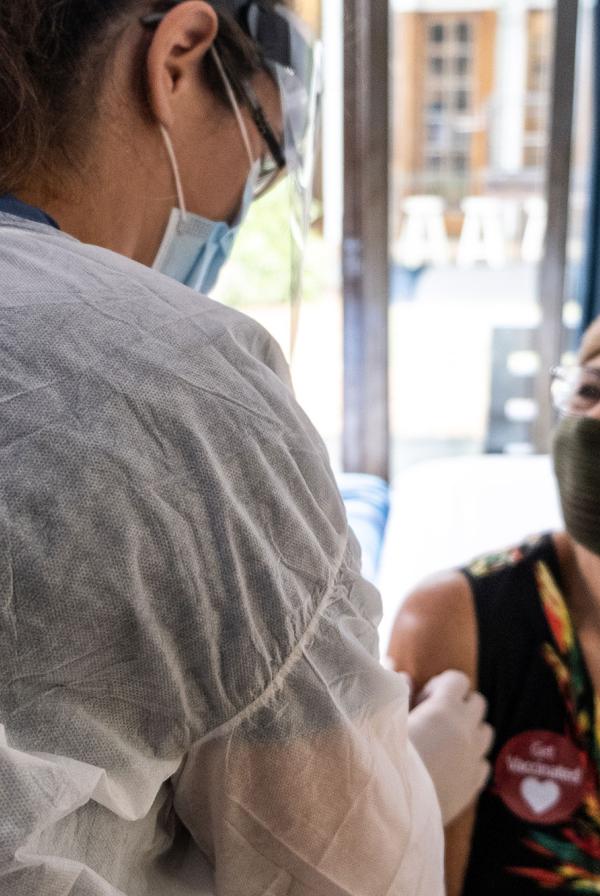
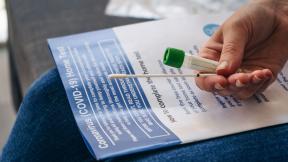
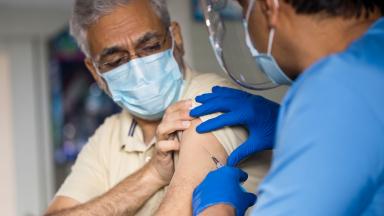
Supporting members through the COVID-19 pandemic, the greatest challenge the health service has faced in its history.
We are actively engaging with developments, representing members' views and focusing our efforts on where they will be greatest use concerning the pandemic.
We are also working with the COVID-19 inquiry team to ensure all experiences from within our complex health and social care landscape are meaningfully represented in the inquiry.